If your private medical practice provides a service, you deserve to be paid accurately and on time....


Medical billing is far more than simply submitting claims to insurance companies. It’s a complex process that involves patient registration, insurance verification, coding, claim submission, payment posting, and denial management. When any part of this process breaks down, it can impact your revenue, your staff workload, and even the patient experience.
For private practices, especially those managing billing internally, the challenge often comes down to workflow visibility, staffing constraints, and evolving payer requirements.
Below are practical medical billing tips and guidelines to help private practices streamline their revenue cycle, reduce denials, and maintain financial stability.
One of the most common misconceptions about medical billing is that it begins and ends with submitting insurance claims.
In reality, billing success depends on the entire revenue cycle management (RCM) process, including:
Problems at the front end of the process, such as incorrect patient information or missing authorizations, often lead to denied claims later.
Audit your workflow regularly to identify where errors most often occur. Many practices discover that billing problems actually start during intake or scheduling.
Front-end errors are one of the largest drivers of claim denials in private medical practices.
Common issues include:
These mistakes delay reimbursement and create extra administrative work for staff.
Shoot for a standard workflow in which insurance verification and authorization checks happen before the patient visit whenever possible.
This proactive step can significantly reduce the number of denied claims and improve cash flow.
Coding errors are another major source of billing delays and compliance risks.
Medical billing depends on the precise use of Current Procedural Terminology (CPT) codes to accurately represent the services provided.
Even small mistakes, such as using an outdated CPT code or omitting the required modifiers, can trigger claim rejections or audits from insurance carriers.
Best practices include:
Accurate coding ensures your practice is reimbursed appropriately for the care delivered.
Many practices struggle with billing simply because they lack clear reporting and performance visibility.
Without reliable reporting, it’s difficult to answer important questions such as:
Transparency in billing reporting allows practice owners and administrators to identify problems early and make informed decisions.
Your billing process should provide regular reports on:
This level of visibility helps practices maintain financial stability and continuously improve their revenue cycle.
Staffing shortages are a growing challenge for many medical practices. When billing teams are understaffed or overwhelmed, critical tasks like claim follow-ups and denial appeals often fall behind.
Common staffing-related billing issues include:
Over time, these gaps can create significant revenue leaks.
Evaluate whether your current billing team has the capacity and expertise required to manage your practice’s revenue cycle effectively. If not, consider additional training, process automation, or outside help.
|
Not sure if your medical billing process is truly optimized? Use our full practice checklist to identify gaps, improve workflows, and uncover missed revenue opportunities. |
Denied claims are inevitable in healthcare billing. How quickly you respond determines how much revenue you recover.
Effective denial management requires:
Many practices fail to analyze denial data, leading to the same errors recurring.
Track your top denial reasons by payer. This allows your team to proactively fix issues and reduce future claim rejections.
One of the most overlooked billing problems is slow or inconsistent follow-up on unpaid claims.
Claims that sit in accounts receivable for extended periods are far less likely to be collected.
A best-practice approach includes:
Proactive follow-up ensures that legitimate claims don’t fall through the cracks.
Billing directly affects how patients perceive your practice.
Confusing statements, delayed invoices, or unclear payment expectations can create frustration for patients.
To improve the patient experience:
When billing is handled professionally and transparently, it strengthens patient trust and satisfaction.
Medical billing processes are not one-size-fits-all.
Different specialties have unique coding requirements, payer rules, and reimbursement structures. A billing approach that works for a primary care practice may not work for a surgical specialty, behavioral health practice, or subspecialty clinic.
Working with a billing partner who understands specialty-specific workflows and payer nuances can dramatically improve efficiency and reimbursement outcomes.
A knowledgeable partner can also help practices navigate:
Even well-run billing systems require ongoing evaluation and adjustments.
Practice leaders should periodically review key signs of performance:
Tracking these metrics helps practices identify operational gaps and maintain financial health.
Medical billing plays a critical role in the success of any private practice. When the process is efficient, transparent, and proactive, it supports both financial stability and a better patient experience.
By improving front-end workflows, strengthening denial management, increasing reporting visibility, and ensuring knowledgeable billing support, practices can reduce administrative burdens while improving revenue performance.
For many offices, partnering with an experienced practice management team can help streamline billing operations and allow physicians to focus on what matters most: providing high-quality patient care.


If your private medical practice provides a service, you deserve to be paid accurately and on time....


Healthcare compliance training is a highly important part of any medical organization’s functions....


When the calendar flips, medical practices often feel it immediately. Claim denials increase,...

In a busy practice, the day can feel like it’s running you instead of the other way around. When...

Getting a Texas physician license can feel like a test of patience long before you ever see a...
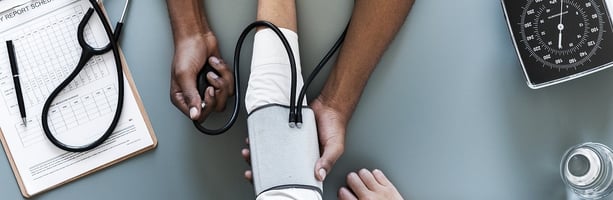
Running a private practice already demands enough from you. Adding hours of administrative work on...
Running a medical practice involves managing dozens of ongoing costs, and understanding them is...

A Texas physician opened a new practice with everything in place – staff hired, patients scheduled,...